How to Get a Sleep Study (At-Home vs Sleep Lab)
If you’ve been waking up exhausted, snoring loudly, or dragging yourself through the day no matter how many hours you spend in bed, an at-home sleep study can be a fast way to get real answers.
Obstructive sleep apnea (OSA) is common and often missed. The American Academy of Sleep Medicine (AASM) estimates about 30 million U.S. adults have OSA, and roughly 80% of cases are undiagnosed.
With today’s home testing and telehealth, you can do a virtual consult, get a portable device mailed to you, and have a board-certified sleep physician review your results without going to a sleep lab.
This guide covers everything you need to know from how home sleep apnea tests work, who qualifies, what the results mean, and how to choose between a home sleep test and an in-lab polysomnography (PSG).

Disclosure: This article is reader-supported and contains affiliate links.
Home Sleep Test vs Sleep Lab – Which to Choose?
Choosing between a home sleep study and an in-lab polysomnography (PSG) depends on your symptoms, health history, and what your doctor suspects is causing your sleep disruptions.
For most otherwise healthy adults with classic obstructive sleep apnea (OSA) signs, a home sleep test is usually enough to confirm OSA and move straight into treatment.
An in-lab sleep study collects broader data and is usually the better choice when symptoms suggest another sleep disorder or there are complicating medical conditions.
A home sleep test is typically a good first step if you:
- Have classic OSA symptoms (loud snoring, witnessed pauses, gasping, daytime sleepiness)
- Are an adult without significant heart, lung, or neuromuscular disease
- Want faster results and lower out-of-pocket costs compared to an in-lab study
- Have been screened and approved by a physician or licensed practitioner
- Are comfortable self-applying a simple wearable device at home
An in-lab PSG is usually the better choice if you:
- Need EEG-based testing for another disorder (narcolepsy, REM sleep behavior disorder, periodic limb movement disorder)
- Have significant cardiovascular disease, COPD, or a neuromuscular condition affecting breathing
- Had a home test that was negative or inconclusive, but symptoms persist
If your home test comes back negative but your symptoms persist, don’t dismiss the result as definitive. Mild OSA can be harder to capture on a single night, and severity can vary. In that situation, an in-lab study is often the next step.
If you checked most of the “home test” boxes above, you’re likely a good candidate.
Lofta’s at-home sleep apnea test includes a telehealth consult plus physician-reviewed results, and costs a fraction of the $1,000 to $7,000 you’d pay for an in-lab study without insurance.
See If You Qualify for Lofta’s At-Home Test →How to Get a Home Sleep Test in 5 Easy Steps
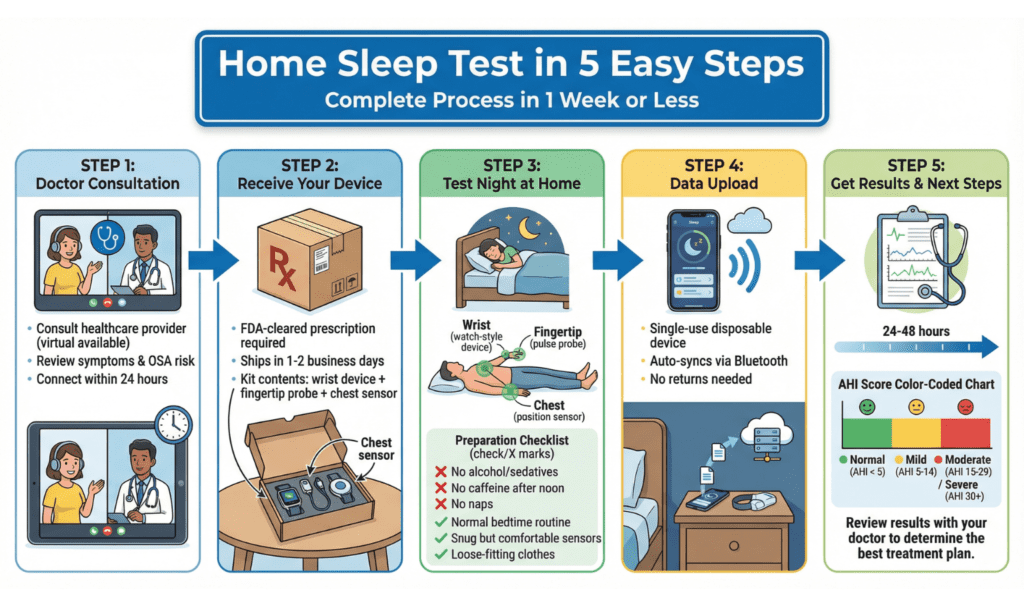
Getting a home sleep test is far simpler than many people expect. From your first conversation with a provider to receiving your sleep report, the process can often be completed within 5-10 days.
1. Schedule a Visit with a Provider
Your first step is a consultation with a licensed healthcare provider such as your primary care doctor, a nurse practitioner, a physician assistant, or a sleep specialist. They’ll review your symptoms and risk factors and decide if a home sleep apnea test is appropriate.
Many providers now offer this initial consultation virtually, eliminating the need for an in-person office visit. Telehealth platforms specializing in sleep health can connect you with a qualified provider quickly.
With Lofta, this step is a short telemedicine video visit to confirm you are a good candidate before anything ships.
2. Secure Your Prescription and Get Your Device
In the U.S., home sleep apnea tests used for diagnosis are prescription medical devices cleared for clinical use. A licensed healthcare provider must order the test. You cannot purchase a clinically approved diagnostic sleep test over the counter.
Once approved, the provider issues the order and the device ships to you. With Lofta, the WatchPAT One typically arrives within a few days after your consultation. The kit includes everything you need to run the test at home (wrist-worn device, chest sensor, and fingertip probe), without complicated setup.
3. Preparing and Using the Equipment at Home
On test night, setup is fairly straightforward. The WatchPAT One uses just three contact points:
- A wrist-worn device (similar in size to a fitness tracker)
- A fingertip uPAT probe to measure peripheral arterial tone, SpO2, and pulse rate
- A chest RESBP sensor to detect snoring, body position, and chest movement
There is no nasal cannula and no bulky effort belts. Simply sleep in your own bed, in your usual position. The familiar setting can make the night feel more comfortable and natural than a sleep lab.
Follow these preparation guidelines on the night of your sleep study to ensure clean, reliable data:
- Avoid alcohol and sedatives that night since they can change breathing
- Skip caffeine after noon on the day of the test
- Don’t take a nap in the afternoon
- Stick to your normal bedtime routine and sleep position
- Ensure all sensors are snug but comfortable before lights out
- Wear loose-fitting clothing that won’t interfere with the chest sensor
4. Upload the Data and Dispose of the Device
The Lofta WatchPAT One is a single use device, so there is nothing to return. The WatchPAT app sends your overnight data by Bluetooth, so the physician can review it soon after you finish the test.
5. Review Results With a Healthcare Provider and Discuss Next Steps
After a board-certified sleep physician reviews your recording, you’ll receive a sleep report.
The primary diagnostic metric is the Apnea-Hypopnea Index (AHI) which is the average number of apnea and hypopnea events per hour of estimated sleep time. Your report will also include the Oxygen Desaturation Index (ODI), snoring statistics, and body position data.
| AHI Score | Severity Classification | Typical Next Step |
| Less than 5 events/hour | Normal (No OSA) | Discuss other causes of symptoms with your doctor |
| 5–14 events/hour | Mild OSA* | Lifestyle changes, positional therapy, possible oral appliance |
| 15–29 events/hour | Moderate OSA | CPAP therapy typically recommended |
| 30+ events/hour | Severe OSA | CPAP therapy strongly indicated; possible in-lab follow-up |
*Note: Per AASM clinical guidelines, an AHI of 5–14 is diagnostic for mild OSA only in patients who have symptoms (such as daytime sleepiness or witnessed apneas). An AHI of 15 or above is diagnostic regardless of symptoms.
Your sleep physician will interpret your AHI score in the context of your specific symptoms and health history. A normal result doesn’t automatically rule out a sleep disorder. If your symptoms remain strongly suggestive of OSA, a follow-up in-lab study may still be warranted.
Most providers deliver results within three to seven days of receiving device data. Lofta’s platform and the WatchPAT One’s auto-upload feature often enable turnaround within 24 to 48 hours of test night.

How to Get an In-Lab Sleep Study (PSG)
If your symptoms or health history point to something beyond straightforward sleep apnea, an in-lab polysomnography (PSG) may be recommended.
The way it works may look like this:
- Talk to your primary care doctor or a sleep specialist. Explain symptoms like snoring, witnessed pauses, excessive daytime sleepiness, unusual nighttime movements, or extreme sleepiness despite enough time in bed.
- Get a referral to a sleep center. Some plans require this step.
- Insurance authorization. Many insurers require pre-authorization for in-lab PSG.
- Complete the overnight study. PSG records EEG brain activity along with signals like oxygen levels, airflow, breathing effort, heart rhythm, and movement.
- Review results and treatment plan. In some cases, CPAP titration can be started the same night if severe apnea is seen.
Who Is a Good Fit for Home Sleep Testing?
Not every patient is a good candidate for an at-home sleep apnea test. A provider will consider your symptoms, medical history, and overall risk before deciding whether home testing is appropriate or whether you should go straight to a sleep lab.
Home sleep testing is often a good fit if you:
- Have loud chronic snoring, witnessed pauses, gasping, or choking episodes
- Feel excessively sleepy during the day despite enough time in bed
- Wake with headaches, dry mouth, or sore throat
- Have high blood pressure or other common OSA risk factors
Home sleep tests may not be appropriate if you:
- Have moderate-to-severe heart disease, heart failure, or complex arrhythmias
- Have COPD or other significant lung disease
- Have a neuromuscular condition that affects breathing
- Have symptoms suggesting another sleep disorder that requires EEG-based testing
- Had a previous negative or inconclusive home test despite strong symptoms
- Are a child (pediatric sleep evaluation is typically done in-lab)
It’s always best to talk with a qualified health professional if you are unsure.
Types of Home Sleep Tests (Type 3, Type 4, and PAT)
Here are the categories most home sleep studies fall into:
Type 3 Devices
Type 3 devices are the traditional standard for diagnosing OSA at home. They typically monitor signals like airflow, breathing effort, oxygen saturation (SpO2), and heart rate. Insurance plans typically cover Type 3 devices when ordered by a physician or licensed practitioner.
Type 4 Devices
Type 4 devices are simpler and often measure only one or two signals, commonly SpO2 via a fingertip pulse oximeter. They’re useful for initial screening but generally aren’t sufficient for a formal OSA diagnosis on their own.
PAT Devices (WatchPAT)
Peripheral Arterial Tonometry (PAT) devices detect sleep apnea events using signals related to arterial tone changes that occur with breathing disruptions
The WatchPAT One, used by Lofta for at-home sleep apnea testing, is a PAT based option that is FDA cleared and accepted for DOT and FMCSA commercial driver testing.
Unlike many traditional Type 3 home sleep test devices, it does not require a nasal cannula or chest effort bands.
Not sure which type of test you need?
Lofta’s telehealth consult walks you through it. A licensed provider reviews your symptoms and confirms whether the WatchPAT One is the right fit before anything ships.
Schedule a Telehealth Consult (No Obligation if You Don’t Qualify) →What Does a Home Sleep Test Measure (and What It Can’t Diagnose)
The WatchPAT One used by Lofta measures multiple sleep-related signals during your recording, including PAT signal, heart rate, oxygen saturation, body position, snoring, and movement.
One advantage of WatchPAT is that it can estimate sleep stages like wake, light, deep, and REM using an algorithm based on PAT signals and movement. This can help estimate sleep time more accurately than total recording time.
Important limitation: Home sleep tests do not record EEG brain waves the way an in-lab PSG does. That’s why they are designed for diagnosing obstructive sleep apnea, not conditions that require full EEG-based sleep analysis, such as narcolepsy, REM sleep behavior disorder, or periodic limb movement disorder.
What if You Test Positive?
A positive result (mild, moderate, or severe OSA) is the start of your treatment plan, not a cause for alarm. Your sleep physician will outline a treatment plan based on your AHI score and overall health profile.
Common next steps may include:
- Mild OSA: positional therapy, weight management, or a custom oral appliance (mandibular advancement device).
- Moderate to severe OSA: CPAP therapy is commonly recommended and requires a prescription.
- Complex cases: an in-lab CPAP titration study may be recommended to calibrate pressure settings overnight.
In-Home Sleep Testing: Your Next Steps
Millions of people are living with undiagnosed sleep apnea. They wake up groggy, push through their days on caffeine, and chalk it up to stress or aging. But a properly ordered sleep study can finally clarify what’s going on and point you toward the next right step.
An at-home sleep test is not a replacement for an in-lab polysomnography when a full study is medically necessary. Still, for many adults with common OSA risk factors, home testing is a clinically supported first step. It’s often faster to schedule, far more affordable, and can get you to a diagnosis and treatment plan sooner.
Ready to find out what’s behind your symptoms?
Lofta’s at-home sleep apnea test includes a telehealth consult, a physician-reviewed sleep report, and free retesting if needed. All for $189 with free shipping. No sleep lab visit, no insurance headaches, and most people have their answers within a week.
Get Your Sleep Apnea Answers in 5–10 Days (No Sleep Lab Required) →Commonly Asked Questions
How to Qualify for an At-Home Sleep Study?
To qualify for an at home sleep study, you typically need symptoms or risk factors for obstructive sleep apnea, such as loud snoring, witnessed breathing pauses, daytime sleepiness, or high blood pressure.
A licensed healthcare provider must evaluate you and determine that home testing is appropriate. It is typically recommended for adults with suspected moderate to high risk OSA and without complex medical conditions.
Is a Prescription Required for a Home Sleep Test?
Yes. In the United States, home sleep apnea tests used for diagnosis are FDA-cleared prescription medical devices. They must be ordered by a licensed healthcare provider.
Can a Home Sleep Test Detect Conditions Other Than Sleep Apnea?
No, home sleep studies can’t detect other conditions. And this is one of the most important limitations to understand. Home sleep tests do not record brain wave activity (EEG), which means they cannot diagnose sleep disorders that require sleep stage analysis.
Conditions requiring a full in-lab polysomnography for accurate diagnosis include:
- Narcolepsy and idiopathic hypersomnia
- REM sleep behavior disorder
- Periodic limb movement disorder (PLMD)
- Restless leg syndrome (RLS) with significant sleep disruption
- Parasomnias such as sleepwalking or night terrors
If your symptoms go beyond snoring and daytime sleepiness, particularly if you experience unusual nighttime movements, vivid dream enactment, sudden muscle weakness, or extreme sleepiness regardless of sleep duration then discuss these specifically with your doctor before assuming a home sleep test will provide complete answers.
Does Insurance Cover a Home Sleep Test?
Coverage depends on your plan and whether testing is medically necessary. Medicare covers certain home sleep apnea tests when ordered by a treating practitioner and performed using an FDA-cleared device. Private plans vary and may require pre-authorization.
Note: Lofta does not bill insurance directly. Reimbursement depends on your insurer.
Without insurance, Lofta’s home sleep test is priced at $189 which is a fraction of the $1,000 to $7,000 you might pay for an in-lab polysomnography without coverage. Free shipping is included, and if Lofta’s medical team determines a retest is clinically needed due to data quality issues, that retest is provided at no additional charge.
Can You Do a Sleep Study at Home for Narcolepsy?
A standard at-home sleep apnea test cannot diagnose narcolepsy. Narcolepsy requires specialized testing such as an overnight in-lab study followed by a Multiple Sleep Latency Test (MSLT), which measures how quickly you fall asleep and enter REM.
How Much Does an At-Home Sleep Study Test Cost?
An at-home sleep study typically costs between 150 and 500 dollars without insurance. In-lab studies often range from 1000 to 7000 dollars or more without insurance, depending on the facility and what is included.
What is Commonly Mistaken for Sleep Apnea?
Conditions often mistaken for sleep apnea include chronic insomnia, anxiety, depression, restless leg symptoms, and simple sleep deprivation. Thyroid disorders and certain heart or lung conditions can also cause fatigue and poor sleep. A proper medical evaluation helps sort out the real cause.
How Many Hours of Sleep Do You Need for an At-Home Sleep Study?
Most providers look for at least 4 hours of usable recording time during an at home sleep study. That does not mean you must sleep perfectly for 8 hours, but longer recording times usually give more reliable data. If there is not enough data, the test may need to be repeated.
What are the Disadvantages of Home Sleep Testing?
The main disadvantages of home sleep testing is that it collects fewer data channels than an in-lab PSG and does not record EEG brain waves. It may miss mild OSA in some cases and cannot diagnose disorders that require EEG-based monitoring.
Health Disclaimer: This information is for educational purposes only and is not medical advice. It does not replace evaluation, diagnosis, or treatment by a licensed healthcare professional. Sleep apnea testing and treatment decisions should always be made in consultation with a qualified provider who can consider your individual symptoms, medical history, and risk factors. If you think you may have a sleep disorder or another medical condition, seek personalized guidance from a licensed clinician.

Sleep Essentials Hub is a sleep blog for readers who want helpful sleep guides and honest product recommendations. We’re passionate about better rest, with a focus on pillows and bedding, sleep aids, sleep apnea and CPAP gear, natural sleep supplements, sleep tech, and simple ways to improve your sleep environment. We’re here to help you choose products that support deeper sleep, greater comfort, and a better night’s rest without overspending.
